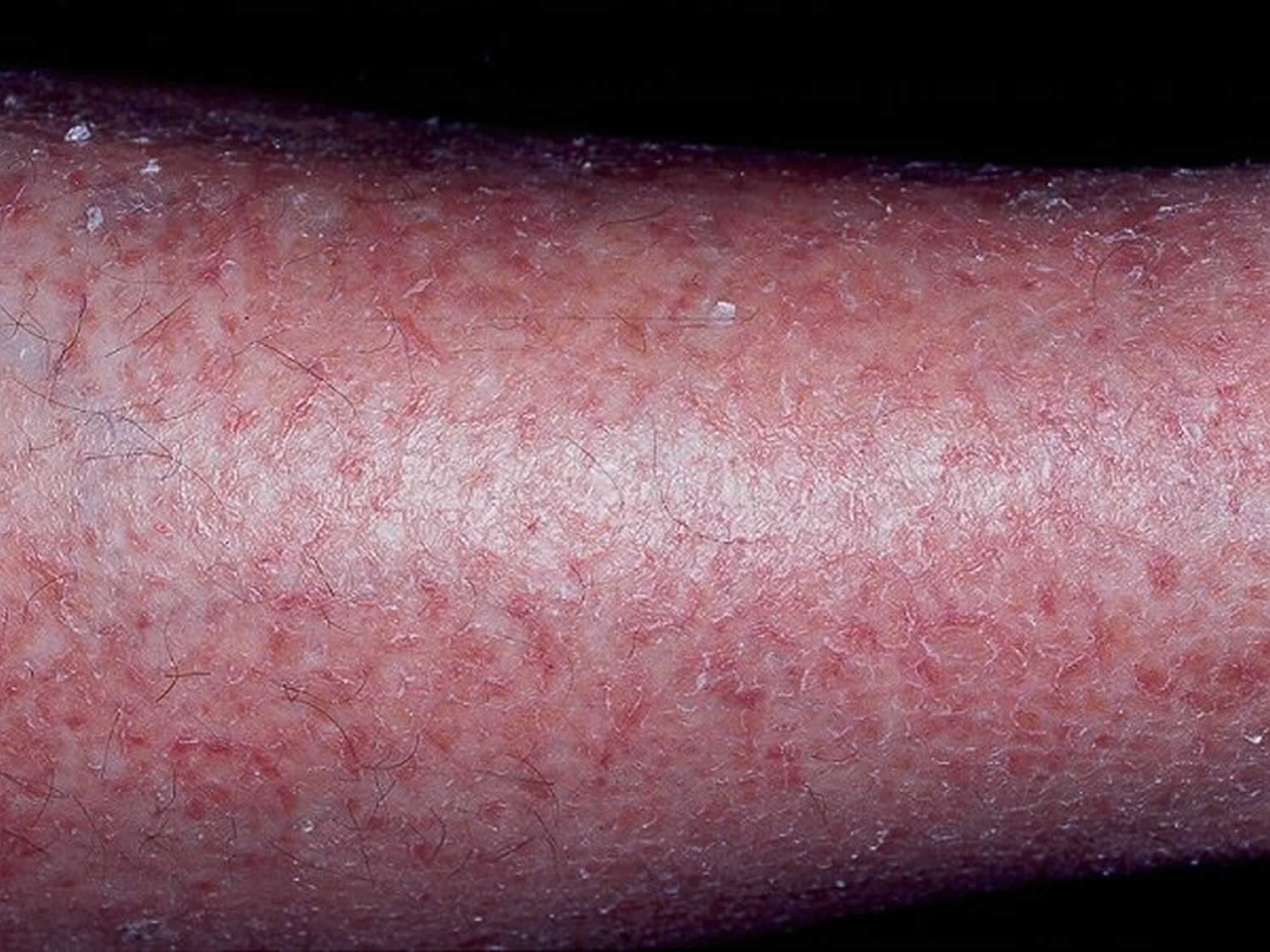
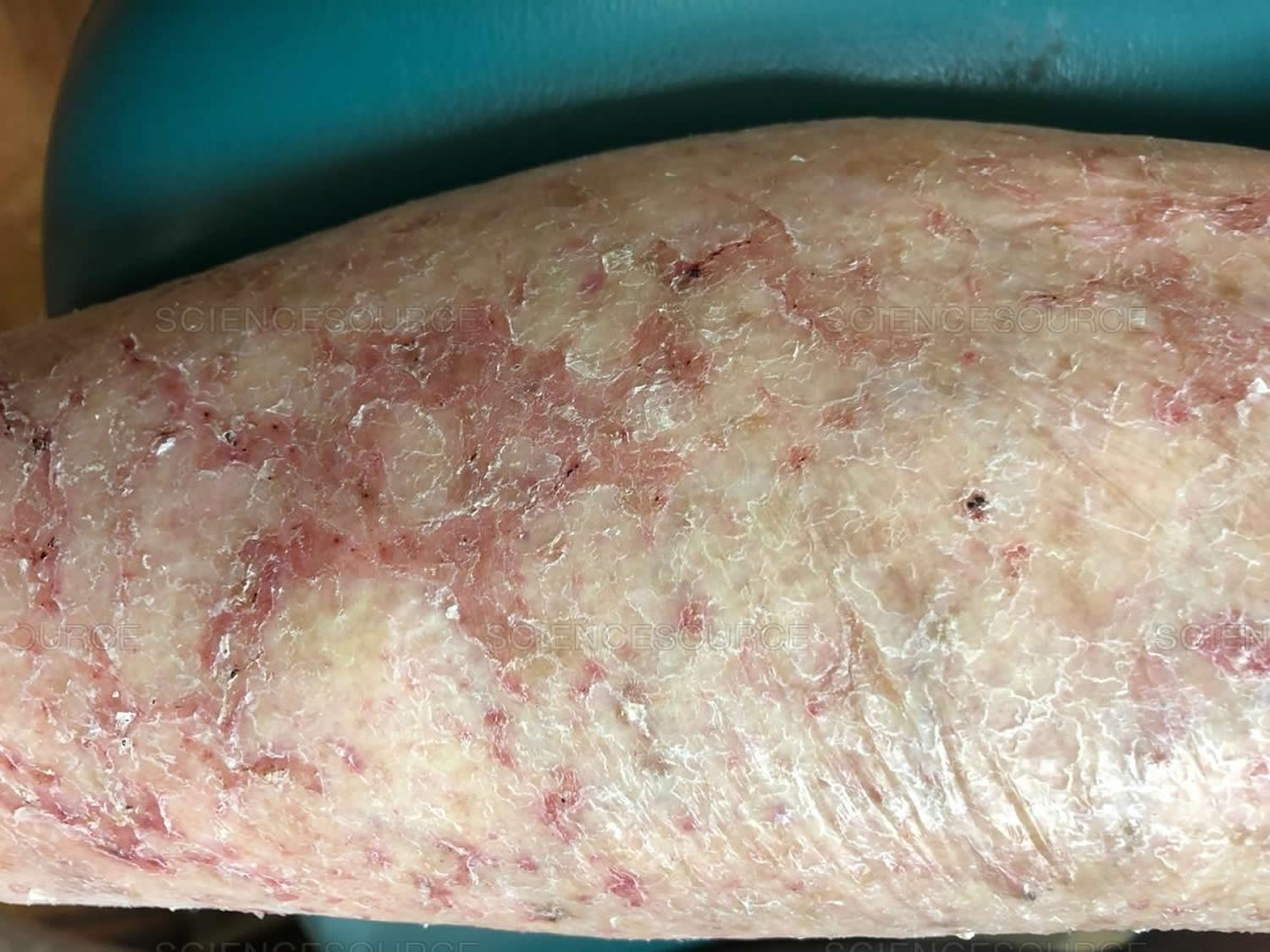
Xerotic eczema
Xerotic eczema also called xerotic dermatitis, asteatotic eczema or dry skin dermatitis, is a common type of dermatitis or eczema that occurs as a result of dry skin. Xerotic eczema got its French name eczema craquelé from its cracked appearance. Xerotic eczema is characterized by itchy, dry, cracked, and polygonally fissured skin with irregular scaling 1. Xerotic dermatitis is precipitated by the drying effect of a cold winter or excess washing. Xerotic eczema most commonly occurs on the shins of elderly patients, but it may occur on the hands and the trunk. Seasonality is prominent, and most patients present in the winter months, especially in areas where indoor humidity is decreased by heating. The frequency of xerotic dermatitis is increased in the northern United States, particularly during the winter season.
Xerotic eczema can occur in anyone with very dry skin, but it most often affects older people. Men older than 60 years develop xerotic dermatitis more commonly than women. The median patient age at presentation is 69 years. Xerotic eczema is also a complication of inherited and acquired forms of ichthyosis. Systemic causes include underactive thyroid (myxedema), malnutrition (zinc and fatty acid deficiencies), severe weight loss and lymphoma. Drugs can cause xerotic eczema, particularly retinoids (acitretin, isotretinoin), diuretics and protein kinase inhibitors.
Xerotic eczema usually rapidly responds to treatment. The following methods may help improve your xerotic eczema 2:
- Eliminate or reduce the use of soap on the involved areas; use soap only in your groin area and armpits.
- Avoid harsh skin cleansers.
- Bathing should be restricted to twice a week and the emollients should be used as a wash as opposed to a soap.
- Apply ointment based emollients following bathing, and use moisturizing agents liberally.
- Apply topical steroid ointments with or without polyethylene occlusion. Note that steroids can thin the cutaneous barrier and lower the threshold for further insults that lead to dermatitis, especially in elderly patients.
- Wool clothing should not be worn over affected areas.
- Use humidifiers.
For particularly inflamed or severe disease, soaking and smearing may be instituted for 1-2 weeks to gain control of the condition 3.
If xerotic eczema persists despite therapy, behavioral changes, and treatment compliance, allergic contact dermatitis and irritant contact dermatitis and internal malignancy may require investigation.
Figure 1. Xerotic eczema
What are emollients and moisturizers?
Emollients are products used to soften skin. Moisturizers are products used to add moisture to the skin. There are numerous emollients and moisturizers on sale at general stores and pharmacies. Options include:
- Oils
- Lotions
- Creams
- Ointments.
Active ingredients of emollients and moisturizers are occlusives and humectants. They often include other ingredients, such as surfactants (non-soap cleansers), fragrances and preservatives.
Emollients and moisturizers are most effective when applied immediately after bathing but can also be applied at other times.
Note: People with sensitive skin associated with atopic dermatitis or rosacea often describe irritant reactions to emollients and moisturizers such as burning and stinging. If irritation is transient, the product can continue to be used. It should be discontinued if contact dermatitis appears.
Occlusive moisturizers
Occlusives are oils of non-human origin, often mixed with water and an emulsifier to form a lotion or cream. They provide a layer of oil on the surface of the skin to reduce water loss from the stratum corneum.
- Bath oil deposits a thin layer of oil on the skin upon rising from the water.
- Lotions are more occlusive than oils.
- Creams are more occlusive again. Thicker barrier creams containing dimethicone are particularly useful for hand dermatitis.
- Ointments are the most occlusive and include pure oil preparations such as equal parts of white soft and liquid paraffin or petroleum jelly.
The choice of occlusive emollient depends upon the area of the body and the degree of dryness and scaling of the skin.
- Lotions are used for the scalp and other hairy areas and for mild dryness elsewhere
- Creams are used when more emollience is required.
- Ointments are prescribed for dry, thick, scaly areas, but many patients find them too greasy.
Sorbolene and glycerine cream is a general-purpose moisturizer that is non-greasy, cheap and available in bulk without prescription.
The minimum quantity for an occlusive emollient is 250 g (or ml) and often 500 g or 1 kg is needed: liberal and regular usage is to be encouraged. How frequently it is applied depends on how dry the skin is: very dry skin may benefit from a greasy emollient every couple of hours, but slightly dry skin may only need a light moisturizer at night.
Humectants
Humectants increase the water holding capacity of the stratum corneum. They include:
- Glycerine
- Urea
- Alpha hydroxy acids such as lactic acid or glycolic acid.
- Salicylic acid
Urea and the acidic preparations often sting if applied to scratched or fissured skin. They are also keratolytic, ie they have a descaling or peeling effect, important in the management of ichthyosis.
Xerotic eczema causes
Xerotic eczema is mainly due to water loss from the stratum corneum. This occurs because of a breakdown of the skin barrier due to genetic predisposition and injury by environmental factors. These include:
- Low humidity (winter, desert, high altitude, travel, use of dehumidifier or fan heater)
- Excessive bathing especially using soaps and detergents.
Xerotic eczema is also a complication of inherited and acquired forms of ichthyosis.
The inherited forms of ichthyosis are due to loss of function mutations in various genes:
- Ichthyosis vulgaris (FLG gene).
- Recessive X-linked ichthyosis (STS gene)
- Autosomal recessive congenital ichthyosis (ABCA12, TGM1, ALOXE3 genes)
- Keratinopathic ichthyoses (KRT1, KRT10, KRT2 genes)
Acquired ichthyosis may be due to:
- Metabolic factors: thyroid deficiency
- Illness: lymphoma, internal malignancy, sarcoidosis, HIV infection
- Drugs: nicotinic acid, kava, protein kinase inhibitors (eg EGFR inhibitors), hydroxyurea.
Systemic causes include underactive thyroid (myxedema), malnutrition (zinc and fatty acid deficiencies), severe weight loss and lymphoma. Drugs can cause xerotic eczema, particularly retinoids (acitretin, isotretinoin), diuretics and protein kinase inhibitors.
Multiple more uncommon etiologic factors may coexist to cause xerotic dermatitis, including the following:
- Decreased keratin synthesis in elderly persons
- Radiation
- Long-term malabsorption of essential fatty acids, including linoleic acid and linolenic acid
- Nutritional deficiencies – Zinc deficiency 4; essential fatty acid deficiency, such as linoleic acid deficiency or linolenic acid deficiency
- Thyroid disease – Myxedema and other thyroid diseases with diminished sweat and sebaceous gland activity 5
- Neurologic disorders – Decreased sweating in denervated areas
- Drugs – Antiandrogen therapy 6 and diuretic therapy
- Malignancies – Malignant lymphoma 7, gastric adenocarcinoma 8, glucagonoma, angioimmunoblastic lymphadenopathy 9, breast cancer, large-cell lung carcinoma, and colorectal carcinoma 10
Xerotic eczema differential diagnosis
Xerotic eczema differential diagnoses include:
- Allergic Contact Dermatitis
- Cellulitis
- Irritant Contact Dermatitis
- Nummular Dermatitis
- Stasis Dermatitis
- Thrombophlebitis
Xerotic eczema symptoms
Xerotic eczema often has a distinctive crazy-paving appearance. Diamond-shaped plates of skin are separated from each other by red bands forming a network. There may also be scratch marks. It may start on one shin but soon spreads to affect the skin around both lower legs.
During the winter months, an elderly person classically presents with itchy and dry skin (xerosis) with dermatitis on the pretibial areas. Sometimes, the dysesthesia may be described as a pinprick or biting sensation.
Severe xerotic eczema can lead to more severe secondary dermatitis with generalized redness, localized swelling and surface blistering. Like other forms of eczema on the lower leg, it can eventually result in widespread secondary disseminated eczema (autosensitization).
Xerotic eczema diagnosis
Xerotic eczema is diagnosed by its appearance and tests are unnecessary in the majority of patients.
Asking the patient about pertinent controllable factors, such as the following, is important:
- Frequency of bathing, showering, and cleansing, and which soaps and cleansers are in contact with the skin
- Types of skin lubricants used, and method and frequency of application
- Diet
- Medications
- Types of clothing worn (Wool may cause irritation.)
- The source, the type, and the temperature of heat that may alter the humidity of the environment
Thyroid function tests are appropriate if there are other signs to suggest hypothyroidism, such as dry, thinning hair, weight gain, lethargy and slowness. If xerotic eczema is of recent onset and accompanied by excessive scaling (acquired ichthyosis), weight loss, fevers or general malaise, the patient should be thoroughly investigated for an internal cause.
Xerotic eczema treatment
Xerotic eczema usually rapidly responds to treatment.
- Consider factors that have caused dry skin: bathe less frequently, use a cream cleanser instead of soap, do not expose skin to direct heat.
- Apply thick emollients and moisturizers such as petroleum jelly/petrolatum or oily cream several times daily — after a few days, thinner ones such as non-ionic cream should be adequate.
- Apply mild topical steroid cream or ointment to reddened skin for a few days; hydrocortisone cream or ointment is often sufficient.
- A more potent topical steroid may be necessary if the eczema is severe.
Ensure the skin is not allowed to dry out again, as xerotic eczema is very likely to recur.
Note that steroids can thin the cutaneous barrier and lower the threshold for further insults that lead to dermatitis, especially in elderly patients.
If xerotic eczema persists despite therapy, behavioral changes, and treatment compliance, allergic contact dermatitis and irritant contact dermatitis and internal malignancy may require investigation.
Medication
Topical steroid ointments with 24- to 48-hour occlusion with polyethylene or Unna boots are the treatment of choice for the rapid resolution of xerotic dermatitis 11. Unna boots with steroid cream or ointment add to therapeutic efficacy and ease of care, especially in the nursing home population. Boots can be left intact usually for 3-5 days. Many patients heal with mild topical steroids (class III-VI) alone, depending on the severity of the xerotic dermatitis, the patient’s compliance with treatment, and the reduction in the use of soap and hot water to the involved areas. Several studies have reported on the successful use of pimecrolimus or tacrolimus cream in conditions other than atopic dermatitis, including seborrheic dermatitis and xerotic eczema, among others. However, more research is needed to clarify the role of topical calcineurin inhibitors in treating these other disorders 12.
The liberal use of moisturizers, especially petrolatum-based preparations, alone or in combination with topical steroids for mild cases of xerotic dermatitis is recommended.
The soak-and-smear method of hydrating the skin by bathing or soaking the affected area followed by immediate application of steroid ointment once daily has been shown to clear more that 90% of patients in 4-14 days. This is best performed at night 3.
Xerotic eczema prognosis
Xerotic eczema responds well to therapy; however, if the causative factors are not eliminated, recurrences are common. Although most cases resolve without ill effects, xerotic eczema can be chronic with relapses frequent during the winter months and during times of low humidity.
References- Asteatotic Eczema. https://emedicine.medscape.com/article/1124528-overview
- Lazar AP, Lazar P. Dry skin, water, and lubrication. Dermatol Clin. 1991 Jan. 9(1):45-51.
- Gutman AB, Kligman AM, Sciacca J, James WD. Soak and smear: a standard technique revisited. Arch Dermatol. 2005 Dec. 141(12):1556-9.
- Weismann K, Wadskov S, Mikkelsen HI, Knudsen L, Christensen KC, Storgaard L. Acquired zinc deficiency dermatosis in man. Arch Dermatol. 1978 Oct. 114(10):1509-11.
- Warin AP. Eczéma craquelé as the presenting feature of myxoedema. Br J Dermatol. 1973 Sep. 89(3):289-91.
- Greist MC, Epinette WW. Cimetidine-induced xerosis and asteatotic dermatitis. Arch Dermatol. 1982 Apr. 118(4):253-4.
- Barker DJ, Cotterill JA. Generalized eczéma craquelé as a presenting feature of lymphoma. Br J Dermatol. 1977 Sep. 97(3):323-6.
- Guillet MH, Schollhammer M, Sassolas B, Guillet G. Eczema craquelé as a pointer of internal malignancy–a case report. Clin Exp Dermatol. 1996 Nov. 21(6):431-3.
- van Voorst Vader PC, Folkers E, van Rhenen DJ. Craquelé-like eruption in angioimmunoblastic lymphadenopathy. Arch Dermatol. 1979 Mar. 115(3):370.
- Higgins EM. Eczema craquelé and internal malignancy. Clin Exp Dermatol. 1997 Jul. 22(4):206
- Cappiello L, Miller OF. Occlusive therapy of asteatotic dermatitis. 1990.
- Day I, Lin AN. Use of pimecrolimus cream in disorders other than atopic dermatitis. J Cutan Med Surg. 2008 Jan-Feb. 12(1):17-26.